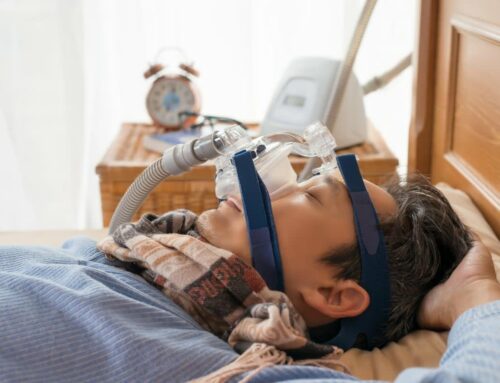
Existe-t-il une relation entre l’apnée obstructive du sommeil (AOS) et les complications cardiovasculaires après une chirurgie majeure non cardiaque?
Dans cette étude de cohorte prospective comprenant 1218 patients à risque subissant une chirurgie majeure non cardiaque, le taux d’événements cardiovasculaires postopératoires (lésion du myocarde, mort cardiaque, insuffisance cardiaque congestive, thromboembolie, fibrillation auriculaire et accident vasculaire cérébral) chez les patients souffrant d’une AOS vs ceux n’ayant pas d’AOS était de 21,7% vs 14,2%, une différence statistiquement significative. Cependant, la différence n’était significative que dans le sous-groupe de patients présentant une AOS sévère.
Matthew TV Chan et al (2019).
Association of Unrecognized Obstructive Sleep Apnea With Postoperative Cardiovascular Events in Patients Undergoing Major Noncardiac Surgery
Importance Unrecognized obstructive sleep apnea increases cardiovascular risks in the general population, but whether obstructive sleep apnea poses a similar risk in the perioperative period remains uncertain.
Objectives To determine the association between obstructive sleep apnea and 30-day risk of cardiovascular complications after major noncardiac surgery.
Design, Setting, and Participants Prospective cohort study involving adult at-risk patients without prior diagnosis of sleep apnea and undergoing major noncardiac surgery from 8 hospitals in 5 countries between January 2012 and July 2017, with follow-up until August 2017. Postoperative monitoring included nocturnal pulse oximetry and measurement of cardiac troponin concentrations.
Exposures Obstructive sleep apnea was classified as mild (respiratory event index [REI] 5-14.9 events/h), moderate (REI 15-30), and severe (REI >30), based on preoperative portable sleep monitoring.
Main Outcomes and Measures The primary outcome was a composite of myocardial injury, cardiac death, heart failure, thromboembolism, atrial fibrillation, and stroke within 30 days of surgery. Proportional-hazards analysis was used to determine the association between obstructive sleep apnea and postoperative cardiovascular complications.
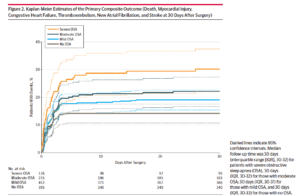
Results Among a total of 1364 patients recruited for the study, 1218 patients (mean age, 67 [SD, 9] years; 40.2% women) were included in the analyses. At 30 days after surgery, rates of the primary outcome were 30.1% (41/136) for patients with severe OSA, 22.1% (52/235) for patients with moderate OSA, 19.0% (86/452) for patients with mild OSA, and 14.2% (56/395) for patients with no OSA. OSA was associated with higher risk for the primary outcome (adjusted hazard ratio [HR], 1.49 [95% CI, 1.19-2.01]; P = .01); however, the association was significant only among patients with severe OSA (adjusted HR, 2.23 [95% CI, 1.49-3.34]; P = .001) and not among those with moderate OSA (adjusted HR, 1.47 [95% CI, 0.98-2.09]; P = .07) or mild OSA (adjusted HR, 1.36 [95% CI, 0.97-1.91]; P = .08) (P = .01 for interaction). The mean cumulative duration of oxyhemoglobin desaturation less than 80% during the first 3 postoperative nights in patients with cardiovascular complications (23.1 [95% CI, 15.5-27.7] minutes) was longer than in those without (10.2 [95% CI, 7.8-10.9] minutes) (P < .001). No significant interaction effects on perioperative outcomes were observed with type of anesthesia, use of postoperative opioids, and supplemental oxygen therapy.
Conclusions and Relevance Among at-risk adults undergoing major noncardiac surgery, unrecognized severe obstructive sleep apnea was significantly associated with increased risk of 30-day postoperative cardiovascular complications. Further research would be needed to assess whether interventions can modify this risk.